Intentionally or not, the healthcare market is doing its best to confuse providers and practice managers, so here is a stab at making sense of it all.
When a practice gets into the business side of medicine, it usually needs to address the following basic needs:
- Keeping the patient’s demographic and insurance information
- Making appointments
- Documenting patient visits and storing the notes
- Filing insurance claims
- Posting payments from insurance companies and patients
- Billing patients
- Keeping up with what is owed and maximizing revenue
There are nuances and additional business activities, but for practices that file insurance claims, these are the basic.
How does this breakdown into the needed systems?
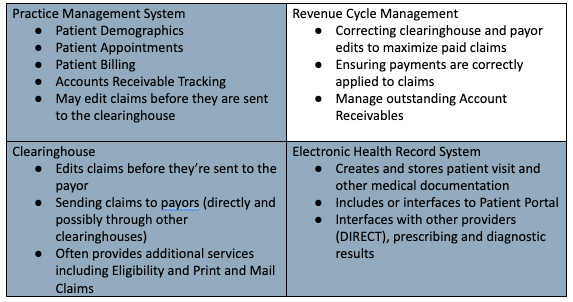
The three blue shaded boxes are typically handled using an automated system. Some vendors separate these components while others package some or all together. Vendors also usually offer additional related services such as:
- Automatic Eligibility Verification
- Appointment Reminders
- Print and Mail Claims (for those that cannot be electronically submitted)
- Print and Mail Statement to Patients
Revenue Cycle Management is an act of managing the practice’s claims process to ensure maximum net revenue. With the advent of EHRs, theoretically, the provider’s coding on the note could flow through to the claim and automatically be sent to the clearinghouse and then onto the payor.
Unfortunately, it is rarely that easy. Providers are not coding experts and trying to turn them into coders reminds me of a southern story about teaching a pig to sing – “it wastes your time and annoys the pig”. So, if you want to maximize your practice’s bottom line you will have someone providing revenue cycle management – either internally or through an RCM service.

