Sevocity Practice Management · Revenue Cycle
Medical Billing Software Built Into Your EHR
Sevocity’s integrated practice management handles your entire revenue cycle (eligibility verification, claims, electronic remittances, and patient billing) without a separate system or a third-party billing service. Fewer touchpoints. Fewer denials. Faster payments.
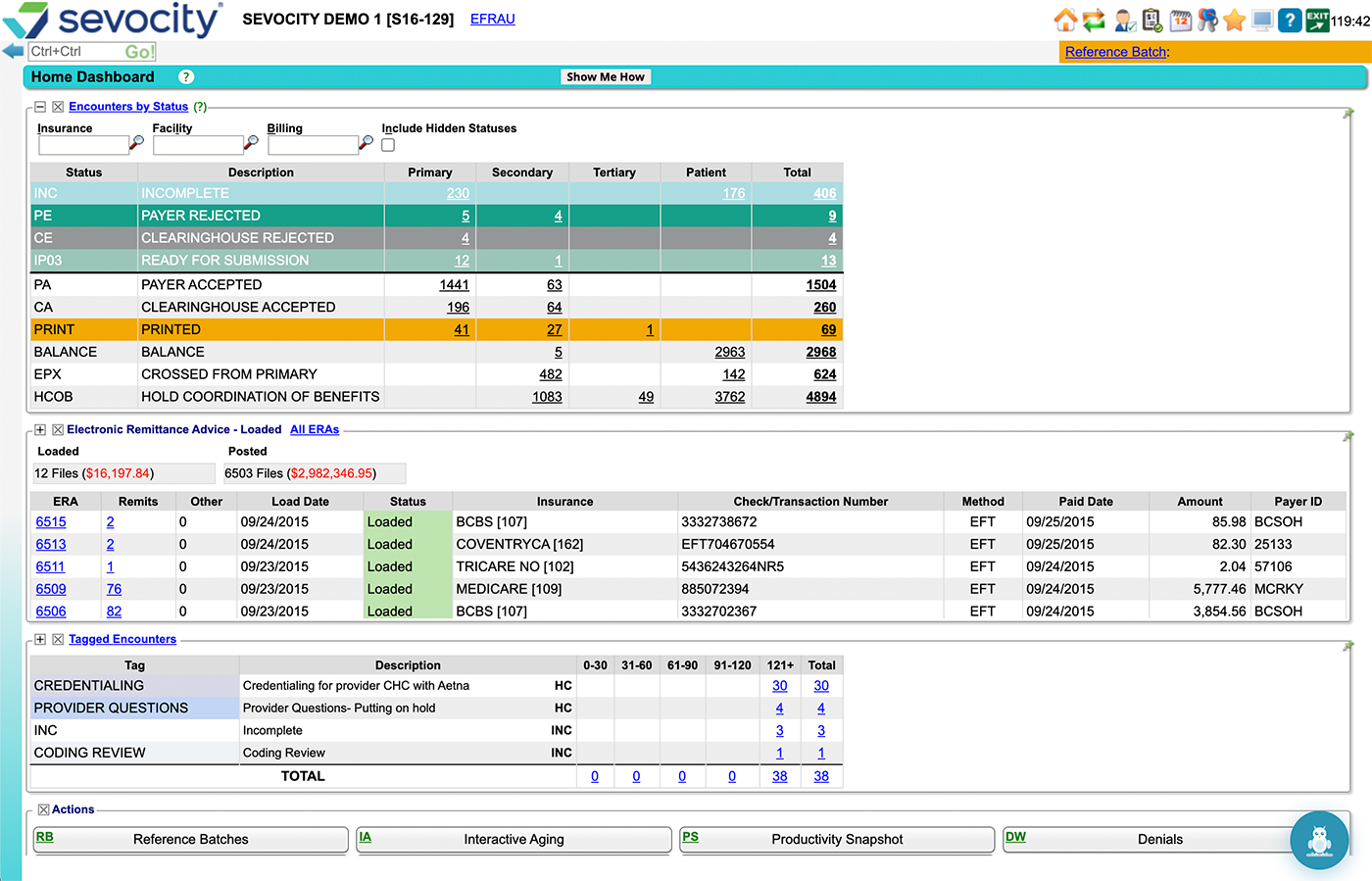
Where Revenue Leaks in Independent Practices
The billing problems most practices treat as inevitable
They’re not inevitable. They’re symptoms of a billing system that isn’t connected to clinical documentation. Sevocity closes that gap.
High Denial Rates
When documentation and billing live in separate systems, coding errors and missing data slip through. Sevocity’s integrated workflow checks eligibility before the visit, scrubs claims before submission, and surfaces denial patterns so you can fix root causes.
Slow Downs in A/R
Manual payment posting, delayed ERA processing, and paper patient statements all extend your collection timeline. Sevocity auto-posts electronic remittances, sends patient statements electronically, and gives you an aging report that updates in real time so nothing sits unworked.
No Visibility into Revenue
If your practice manager pulls a billing report from one system and then logs into the EHR to check visit volume, you’re already behind. Sevocity’s reporting ties clinical activity to financial outcomes. You see collection rates, payer performance, and outstanding A/R without switching tabs.
Revenue Cycle — Feature by Feature
Everything your billing team needs. One system.
Real-Time Eligibility Verification
Verify patient insurance coverage before the visit, automatically, based on the their scheduled appointment. Catch coverage gaps, co-pay information, and authorization requirements before the patient arrives, not after the claim denies.
Claims Management and Scrubbing
Claims generated directly from clinical documentation. No duplicate data entry. Sevocity’s integrated clearinghouse (Etactics) scrubs claims for errors before submission and routes them to the correct payer. Track claim status from submission through payment in a single workflow.
Electronic Remittance and Auto-Posting
Receive ERA files electronically and post payments automatically. No manual entry required for routine remittances. Exceptions and denials are flagged for review. Your billing staff works exceptions, not data entry.
Patient Billing and Online Payments
Send patient statements electronically, accept online payments through the patient portal, and post patient collections directly in the billing system. Reduce paper statements, accelerate patient collections, and give patients a convenient payment option without adding staff time.
Denial Management and Resubmission
Denied claims are flagged immediately with the denial reason and the patient encounter attached. Correct and resubmit from the same screen. No switching between the EHR, clearinghouse portal, and billing system. Track denial patterns by payer and code to address root causes.
Revenue Reporting and A/R Visibility
A/R aging by payer and patient. Collection rates by provider and payer. Denial rates by code. Monthly and year-to-date revenue summaries. Your practice manager runs these reports from Sevocity. No spreadsheet exports, no waiting for your billing service to send a report.
Revenue Clarity, Not Revenue Chaos
Know where every dollar is before you need to ask
Most practice management systems require your biller to run a report, export it, and hand it to the provider or practice owner. By the time the data is in front of the decision-maker, it’s already a week old.
Sevocity’s dashboard gives providers and practice owners direct access to the revenue metrics that matter (A/R aging, payer performance, and month-to-date collections) updated in real time, visible from the same login as clinical documentation.
Access the numbers you need without waiting on a report, whether billing is managed internally or through a trusted billing partner.
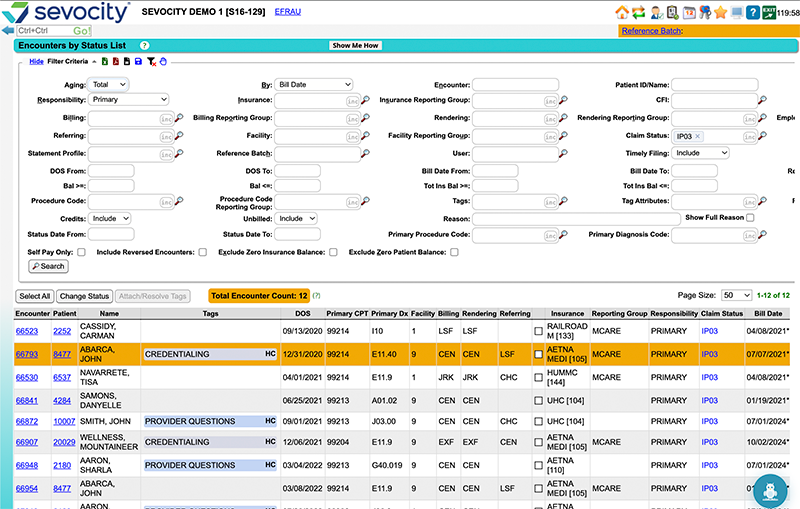
“Sevocity allows for a lot of migrating of information with only a few steps. There was no disruption to our billing or practice flow.”
— Practice Manager, Multi provider family medicine practice · Capterra
Billing Questions
What practices ask about billing before switching EHRs
Yes. Sevocity’s EHR can be used independently from the practice management system. If you have an existing billing service or use a standalone PM system you’re not ready to leave, Sevocity can integrate via standard interfaces. That said, most practices that run both the EHR and PM through Sevocity see the biggest reduction in denials and posting time. The integration removes any rekeying step where errors typically enter.
Sevocity’s integrated practice management uses Etactics as the clearinghouse for claims submission and ERA processing. Etactics has payer connections across major commercial insurers and government payers. Claims route through Etactics automatically. You don’t manage a separate clearinghouse login or reconcile two portals.
When a payer sends an ERA (Electronic Remittance Advice), Sevocity receives it through Etactics and matches payments to the corresponding claims automatically. Payments within expected parameters post without manual entry. Discrepancies (underpayments, denials, or contractual adjustments outside normal ranges) are flagged for your billing staff to review. The goal is for routine payments to post themselves; your biller focuses on exceptions.
Yes. Patients can view and pay their balance through the Sevocity patient portal. Statements can be sent electronically, and payments made through the portal post directly to the patient account in the practice management system. You can still send paper statements for patients who prefer them. The system supports both workflows.
Sevocity’s practice management includes standard revenue cycle reports: A/R aging by payer and patient, collection rate by provider and payer, denial rate by code and payer, charges and payments by date range, and month-to-date and year-to-date revenue summaries. Reports are generated within the system. No export to Excel required for standard analysis. Custom report configuration is available through your Sevocity support team.
See the Full Revenue Cycle in One Demo
Tell us your current billing workflow. Your clearinghouse, your denial rate, how your ERA posting works today. We’ll show you exactly where Sevocity changes the math. 30-minute demo, or 15 minutes focused on billing and A/R.

